In modern medicine, one remarkable advancement has truly transformed the way surgeries are performed – robotic-assisted surgery. Over the past three decades, this cutting-edge technology has left an indelible mark on various surgical specialties, making procedures less invasive and more precise. Today, robotic-assisted surgery is employed across various medical disciplines, from general surgery to otorhinolaryngology.
This article delves into the intriguing history of robotic surgery, explores its myriad benefits, and highlights its application in head and neck surgical procedures, all while considering the factors of cost-effectiveness and patient acceptance.
The Birth of Robotic Surgery
The journey of robotic surgery began in 1985 with the creation of the PUMA 560 – the pioneer robotic surgery system. Initially designed to enhance the accuracy of image-guided intracranial biopsies, this innovation laid the foundation for a medical revolution. In the early 1990s, the ROBODOC system received FDA approval for arthroscopic hip surgery, marking the first instance of a robotic system being employed in medical procedures.
Telepresence Surgery and Technological Advancements
Around the same time, the National Aeronautics and Space Administration (NASA) and Stanford Research Institute (SRI) joined forces to develop telepresence surgery. This groundbreaking concept involved virtually transporting a surgeon from a distant location into the operating theater. As surgeons became well-versed in minimally invasive laparoscopic techniques, they recognized the limitations of rigid equipment and two-dimensional views. To overcome these challenges, semi-rigid robotic equipment with three-dimensional views was developed, leading to innovations like the Automated Endoscopic System for Optimal Positioning (AESOP). AESOP was a robotic arm guided by a surgeon’s voice commands that manipulated an endoscopic camera, significantly improving surgical visualization.
The Rise of the da Vinci Surgical System
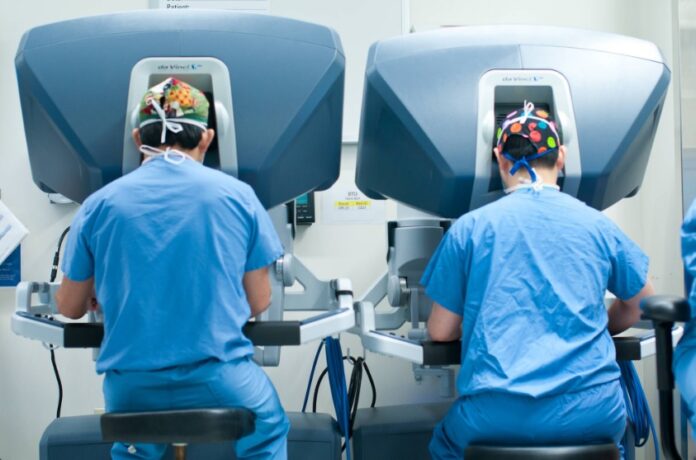
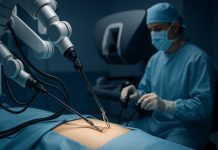
In the world of robotic-assisted surgery, the da Vinci Surgical System has risen to prominence and now stands as one of the most widely used robotic systems. It functions on a master-slave model, with a surgical robotic cart housing multiple control arms that can be remotely operated from a console. The surgical cart includes arms with cameras and EndoWrist instruments that provide exceptional maneuverability, giving surgeons precise control during procedures. This technology incorporates video-assisted visualization, PC enhancement, and a three-dimensional image, offering a depth of perception unparalleled by traditional methods.
Robotic Surgery in Head and Neck Procedures
Robotic-assisted surgery has made significant inroads in head and neck surgical procedures. For instance, in 2001, robots were employed to insert craniomandibular implants for securing silicone ear prostheses onto the skull, reducing surgical complications and enhancing accuracy.
In thyroid surgery, a study conducted in 2007 demonstrated that robotic-assisted bilateral transaxillary endoscopic thyroidectomy (r-baea) was both feasible and safe, with the added advantage of minimal scarring, reduced postoperative pain, and a quicker return to normal activities.
Transoral robotic surgery (TORS) has also been pivotal in treating head and neck cancer. A study conducted in 2009 evaluated functional outcomes in TORS patients, demonstrating positive results with patients resuming oral intake within weeks of surgery.
Robotic Surgery for Oropharyngeal Cancer
Robotic surgery has proven effective in treating oropharyngeal cancer. A study from 2010 reported promising outcomes with a recurrence-free survival rate of 86.5% for patients undergoing transoral robotic-assisted resection. These results underscore the potential of TORS as a primary surgical modality for cancer control.
Treatment of Sleep Disorders
Robotic surgery has even found applications in treating sleep disorders. In 2013, researchers evaluated the efficacy of base of tongue (BOT) resection via TORS in managing obstructive sleep apnea-hypopnea syndrome (OSAHS). The study demonstrated significant improvements in apnea-hypopnea index (AH-i), daytime somnolence, and snoring intensity.
Cost-Effectiveness and Patient Acceptance
While robotic-assisted surgery offers numerous advantages, it’s essential to consider cost-effectiveness and patient acceptance. Studies have shown that robotic surgery can reduce hospital stays, decrease healthcare costs, and result in shorter patient recovery times. Moreover, patients often report higher satisfaction levels due to minimal scarring and reduced postoperative pain.
Conclusion
The history of robotic surgery is one of innovation, progress, and life-changing medical advancements. Robotic-assisted surgery has transformed the healthcare landscape from its humble beginnings with the PUMA 560 to the widespread use of the da Vinci Surgical System. Its applications in head and neck surgery, cancer treatment, and sleep disorder management demonstrate the versatility and potential of this groundbreaking technology. As it continues to evolve, robotic-assisted surgery promises to further improve patient outcomes and revolutionize the surgical field.


![Best hospitals for robotic surgery in India [Updated]](https://roboticsbiz.com/wp-content/uploads/2019/12/surgical-218x150.jpg)
